Sam Barrett, Beronica Garcia, Kristen Levermore,
Luke McGuiness, Maeve O’Dowd Forrestal, Tomasz Pawlak
Contributors
The long winter months are usually spent drinking tea and celebrating Christmas and the New Year. However, it is common for these normally enjoyable periods to be frequently punctuated with nasty colds, flus and “other” problems, with the Centre for Disease Control in the United States recording nearly 7,000 cases of the influenza virus in one week in mid-January last year. But how much do we really know about being sick? A survey of 149 senior freshman Science students at Trinity recently conducted by Prof Cliona O’Farrelly (School of Biochemistry and Immunology) and some of her students (see author list) displayed some remarkable results regarding exactly what students know about sickness.
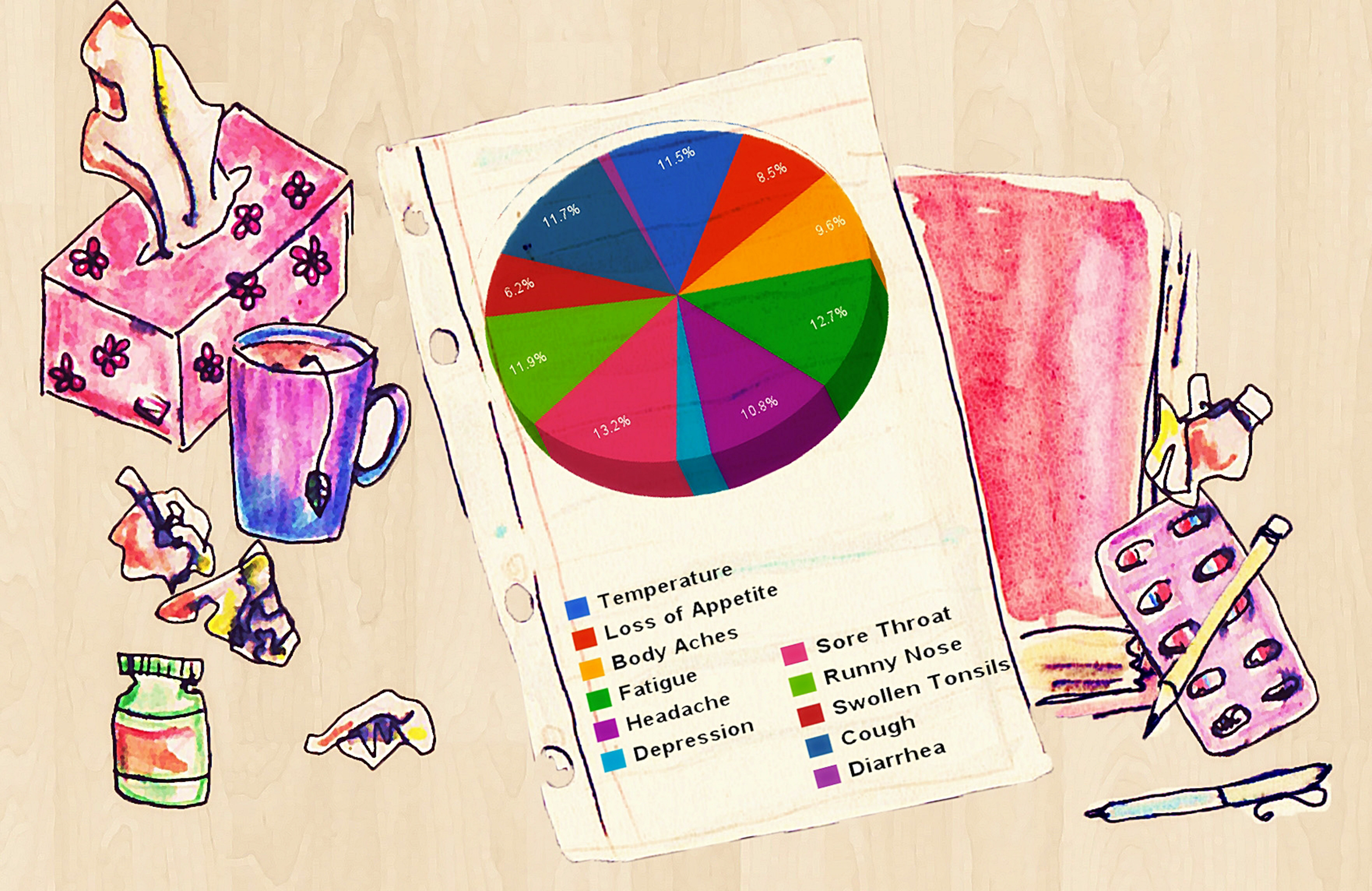
Despite the fact that most sickness in the developed world is caused by either bacteria or viruses, only 32% of students knew if their sickness was due to bacterial or viral infection. This lack of knowledge is likely due to the fact that the differences are so subtle that even most GPs cannot distinguish between them based on symptoms alone, instead requiring expensive in-depth tests with long waiting periods to ensure accurate diagnosis. People will often refuse to wait this long and instead want immediate treatment – which is a problem, when we consider that although symptoms are similar, treatment of bacterial and viral infection is very different. Most bacterial infections or viruses produce similar responses from your body’s immune system. 13.2% of students reported having a sore throat in the last three months, and 11.5% of students recorded having a raised temperature. Both are common to bacteria and virus-induced illness, and the majority of the same students said that they took only generic painkillers and had a day of rest. This trend marks a common attitude in medicine today: the treatment of symptoms, not of the cause. People want to recover and want their symptoms relieved, with very few caring what pathogen it is that they are infected with. It is also important to make a note of stigma associated with certain symptoms.
Depression, for example, is fairly common in humans due to conservation of energy and in the past, hiding away from predators (where we could recover, without getting in harm’s way from them). Not surprisingly, this symptom was one of the least admitted to by the surveyed students – even though the survey was anonymous. It may be that the symptom seems too vague to define and therefore is hard to recall, or that it was simply suffered the least.
But should we care? The most common form of treatment for bacteria is the prescription of antibiotics. Antibiotics strip the body of many of its natural defences in an effort to kill the bacteria causing your illness. Viruses, however, cannot be treated with antibiotics. Viruses have a different molecular structure, method of infecting a host, and of reproducing and cannot be treated as a bacterial infection would be. Despite the two very different causes of illness, one in 20 students were prescribed antibiotics without having a definite diagnosis, with two virus-infected students even saying they had received antibiotics to “prevent” a bacterial infection on top of paracetamol for their current infection. The over-prescription of antibiotics is a common topic in newspapers today, with the overall economic cost and nutrient cost to patients being called into question, as well as emergence of antibiotic resistant bacteria, which is a major concern of the World Health Organisation. In addition, there is a danger that bacteria could one day evolve beyond our common antibiotic treatments, leaving us in a very dangerous place.
“Quite simply, many people do not know what they are infected with and we may only assume that as long as the symptoms are treated, they don’t care about the pathogen in question. Due to the pressure of getting back to health, many people are taking unnecessary antibiotics and this can lead to the evolution of superbugs, such as MRSA.”
But some people don’t get sick. Ever. Out of the population surveyed, it was also noted that there was a great variation between households, in some cases only the participant became ill while in others the entire household succumbed to the bacteria or virus. Why would this happen, what could be the variation? One such possible explanation would be genetics. Each person has a unique set of DNA and so each person’s immune system is slightly different. This phenomenon is accredited to the MHC (major histocompatibility complex), which is the major gene responsible for keeping us healthy. It is a polymorphic gene, meaning that the multiple forms of a single gene that can exist in an individual or among a group of individuals. This variation in our species results in differences in susceptibility, meaning that each person has a different capability for fighting bacteria and viruses.
This phenomenon could be seen in the population surveyed, as 25% of participants reported that only a portion of the total number of people who lived with them were later infected by the same bacterial infection or virus. In such cases, the people in the household would probably be closely related and so would have a similar immune system. However, if you live with an unrelated roommate, the probability of resisting certain infections increases, as your genes could vary greatly, making you less susceptible to catching that disease: not everybody in the residence would be infected by the same pathogen.
So what was the point of all of the group’s head scratching? Quite simply, many people do not know what they are infected with and we may only assume that as long as the symptoms are treated, they don’t care about the pathogen in question. Due to the pressure of getting back to health, many people are taking unnecessary antibiotics and this can lead to the evolution of superbugs, such as MRSA. There is also a genetic aspect to becoming sick. Some people never seem to get colds while others seem to have chronic colds. We are of course not suggesting for a moment that just because you are genetically predisposed to fight off a cold that you will never get one; there are other factors to take into account, general health, stress levels and environment etc. The last, but not least, point this project had was to educate the general college population. If we taught just one person about how we get sick and they realised how certain medications are designed for certain illnesses, then we have done our job as scientists, because after all, knowledge is power.
Viral infections include: All colds and flu, most coughs, most sore throats and usually involve several parts of the body. Bacterial infections include: Strep throat, urinary tract infections, most ear infections, some sinus infections and are usually localized at a single point in the body.